Friday 22 December 2023
COVID JN.1 Variant - Should we worry ?
Tuesday 8 August 2023
Dengue Fever : What should you know ?
Dengue: Symptoms, Prevention, and Treatment**
**Author: Dr. Koushik Debnath, MD (Clinical Microbiology and Infectious Diseases)**
Dengue fever is a viral illness that continues to be a major global health concern, particularly in tropical and subtropical regions. As a specialist in Clinical Microbiology and Infectious Diseases, I find it crucial to shed light on this disease, its symptoms, preventive measures, and available treatments. In this article, we will delve into the nuances of dengue and provide essential information for both the general public and medical professionals.
**Introduction to Dengue:**
Dengue is caused by the dengue virus, which is primarily transmitted to humans through the bites of infected Aedes mosquitoes, particularly Aedes aegypti and Aedes albopictus. This virus is classified into four serotypes, labeled as DEN-1, DEN-2, DEN-3, and DEN-4. Once infected, individuals can develop mild to severe symptoms.
**Symptoms and Clinical Presentation:**
Common symptoms of dengue include high fever, severe headache, joint and muscle pain, skin rash, and mild bleeding. In severe cases, dengue can progress to dengue hemorrhagic fever (DHF) or dengue shock syndrome (DSS), which can lead to bleeding, organ impairment, and even death if not promptly managed.
**Preventive Measures:**
1. **Mosquito Control:** The primary method of preventing dengue is to control mosquito populations. This can be achieved by eliminating standing water where mosquitoes breed, using mosquito nets, and applying insect repellents.
2. **Personal Protection:** Wearing long-sleeved clothing and using mosquito repellents when outdoors can significantly reduce the risk of mosquito bites.
3. **Community Efforts:** Community engagement in maintaining clean surroundings and preventing water accumulation is crucial in minimizing mosquito breeding sites.
**Diagnosis and Treatment:**
Diagnosing dengue involves clinical evaluation, combined with laboratory tests like serological tests and molecular assays. Early detection is essential to prevent severe complications. Unfortunately, there is no specific antiviral treatment for dengue. Management primarily involves supportive care, including hydration, fever-reducing medications, and monitoring for complications.
**Future Directions:**
Efforts to combat dengue include ongoing research into vaccine development. The first dengue vaccine, Dengvaxia, has been approved for limited use in certain regions, but its efficacy and safety have been subjects of debate. Further research is needed to develop effective vaccines that protect against all serotypes.
**Conclusion:**
Dengue remains a significant public health challenge, particularly in regions where Aedes mosquitoes thrive. Education, mosquito control, and community engagement play pivotal roles in preventing and managing dengue outbreaks. As a specialist in Clinical Microbiology and Infectious Diseases, my aim is to create awareness about this disease and emphasize the importance of collaborative efforts in its prevention and control.
Remember, staying informed and taking proactive measures can greatly contribute to reducing the impact of dengue on individuals and communities.
Tuesday 6 June 2023
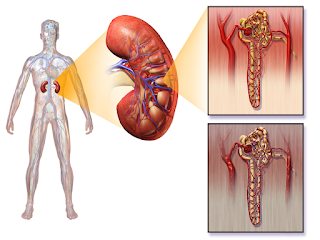
Diabetic Nephropathy: Diagnosis, Management, and Treatment for Optimal Kidney Health
Diabetic nephropathy is a chronic kidney disease that is one of the most common complications of diabetes mellitus. It is characterized by the gradual deterioration of kidney function, leading to proteinuria, hypertension, and eventually end-stage renal disease (ESRD). Early detection, accurate diagnosis, and proper management of diabetic nephropathy are crucial to slow down disease progression and improve patient outcomes. This article aims to provide a comprehensive guide to the diagnosis and management of diabetic nephropathy.
Diagnosis:
1. Screening and Early Detection:
- Regular screening of individuals with diabetes is essential to detect the onset of kidney damage at an early stage.
- Urine albumin excretion rate (AER) and albumin-to-creatinine ratio (ACR) are used to assess albuminuria.
- Estimated glomerular filtration rate (eGFR) is calculated using equations such as the Modification of Diet in Renal Disease (MDRD) or Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI) formula.
- Screening should begin at the time of diabetes diagnosis for type 2 diabetes and within 5 years of diagnosis for type 1 diabetes.
2. Staging and Diagnosis:
- Diabetic nephropathy is staged based on albuminuria and eGFR as per the Kidney Disease: Improving Global Outcomes (KDIGO) guidelines.
- Stages include normoalbuminuria, microalbuminuria, macroalbuminuria, and ESRD.
- Additional tests, such as renal ultrasound and kidney biopsy, may be conducted to evaluate kidney structure and determine the underlying cause.
Management:
1. Glycemic Control:
- Intensive glycemic control through lifestyle modifications, oral hypoglycemic agents, or insulin therapy can significantly delay the onset and progression of diabetic nephropathy.
- HbA1c levels should be maintained below the recommended targets, considering individual patient characteristics and comorbidities.
2. Blood Pressure Management:
- Optimal blood pressure control is vital to slow the progression of kidney disease.
- The target blood pressure goal for most patients with diabetic nephropathy is <130/80 mmHg.
- Lifestyle modifications and antihypertensive medications, including ACE inhibitors (ACEIs) or angiotensin II receptor blockers (ARBs), are commonly prescribed.
3. Proteinuria Management:
- Reducing proteinuria is an essential therapeutic goal.
- ACEIs and ARBs not only control blood pressure but also reduce proteinuria.
- Other agents, such as direct renin inhibitors and aldosterone antagonists, may be considered in resistant cases.
4. Dyslipidemia Management:
- Dyslipidemia is commonly associated with diabetic nephropathy and increases the risk of cardiovascular disease.
- Statins and fibrates are frequently prescribed to manage dyslipidemia and reduce cardiovascular risk.
5. Sodium and Fluid Restriction:
- Dietary sodium restriction is recommended to manage hypertension and fluid retention.
- Fluid intake should be adjusted based on individual patient needs and urine output.
6. Smoking Cessation and Lifestyle Modifications:
- Encouraging smoking cessation and adopting a healthy lifestyle, including regular exercise, weight management, and a balanced diet, are essential components of diabetic nephropathy management.
7. Monitoring and Follow-up:
- Regular monitoring of kidney function, blood pressure, glycemic control, and proteinuria is necessary to evaluate the response to treatment and identify any progression of the disease.
- Patient education and adherence to treatment regimens play a crucial role in achieving optimal outcomes.
Saturday 3 June 2023
Unleashing the Potential of Probiotics: Cultivating Gut Health for Optimal Well-being
Probiotics have emerged as a groundbreaking solution for enhancing gut health and promoting overall well-being. In this article, we will delve into the tremendous potential of probiotics, highlighting their role in nurturing a healthy gut and optimizing our overall physical and mental health. Discover how incorporating probiotics into your daily routine can contribute to a happier and healthier lifestyle.
Section 1: Understanding the Power of Probiotics
Probiotics are live bacteria and yeasts that offer numerous health benefits when consumed in adequate amounts. These beneficial microorganisms play a vital role in maintaining a balanced gut environment, aiding digestion, and supporting immune function.
Section 2: Nurturing Gut Health with Probiotics
By incorporating probiotics into your daily routine, you can create a thriving environment in your gut. Probiotics work by replenishing and restoring the natural balance of beneficial bacteria, which may be disrupted by factors such as poor diet, stress, or antibiotic use. By nurturing your gut health, you lay the foundation for overall well-being.
Section 3: Optimizing Physical Health with Probiotics
Probiotics have been shown to improve various aspects of physical health. They enhance nutrient absorption, aid in weight management, and contribute to a healthy cardiovascular system. Additionally, probiotics can alleviate symptoms associated with gastrointestinal disorders such as irritable bowel syndrome (IBS) and promote regular bowel movements.
Section 4: Boosting Mental Health and Well-being
The gut and brain are intricately connected through the gut-brain axis. Probiotics have been found to influence mental health by modulating the production of neurotransmitters, reducing stress levels, and improving mood. Incorporating probiotics into your diet can be a proactive step towards maintaining a healthy mind and emotional balance.
Section 5: Embracing a Healthier Lifestyle
By harnessing the power of probiotics, you can embrace a healthier lifestyle. Incorporate probiotic-rich foods such as yogurt, sauerkraut, and kefir into your diet. Alternatively, opt for high-quality probiotic supplements to ensure an adequate intake. Combined with regular exercise and a balanced diet, probiotics can contribute to a holistic approach to well-being.
Conclusion:
Probiotics offer a multitude of benefits for nurturing gut health and promoting overall well-being. By understanding the power of probiotics and incorporating them into your daily routine, you can optimize your physical and mental health, paving the way for a happier and healthier lifestyle. Take the proactive step towards harnessing the potential of probiotics and experience the transformative impact they can have on your overall well-being.
Thursday 1 June 2023
"Unveiling the Hidden Dangers: Exploring the Health Risks of Secondhand Smoking"
Unveiling HMPV: A Comprehensive Guide to the Spreading Virus in the US
Introduction:
HMPV, short for Human Metapneumovirus, is a virus that is currently spreading in the United States. It's important to understand what this virus is and how it can affect us. In this article, we will provide you with an easy-to-understand explanation of HMPV and its key characteristics.
1. What is HMPV?
HMPV is a type of virus that primarily affects the respiratory system. It belongs to the same family as the common cold and respiratory syncytial virus (RSV). It was first identified in 2001 and has since been recognized as a common cause of respiratory infections, especially in young children and older adults.
2. How does HMPV spread?
HMPV spreads from person to person through respiratory droplets when an infected individual coughs or sneezes. These droplets can then be inhaled by nearby individuals, leading to infection. It can also spread by touching surfaces contaminated with the virus and then touching the face.
3. What are the symptoms?
The symptoms of HMPV are similar to those of other respiratory infections. They may include cough, runny nose, sore throat, fever, and difficulty breathing. In severe cases, it can lead to pneumonia or bronchiolitis, particularly in young children or individuals with weakened immune systems.
4. Who is at risk?
While HMPV can affect people of all ages, it is more likely to cause severe illness in infants, young children, older adults, and individuals with underlying health conditions. These individuals should take extra precautions to avoid exposure to the virus.
5. How can HMPV be prevented?
Preventing the spread of HMPV involves practicing good hygiene and taking precautions to minimize exposure. Some preventive measures include:
- Washing hands frequently with soap and water for at least 20 seconds.
- Using hand sanitizers if soap and water are not readily available.
- Covering the mouth and nose with a tissue or elbow when coughing or sneezing.
- Avoiding close contact with individuals showing symptoms of respiratory infection.
- Disinfecting frequently-touched surfaces regularly.
6. Is there a specific treatment ?
Rest with supportive care, such as getting plenty of rest, staying hydrated, and using over-the-counter medications to alleviate symptoms. In severe cases, hospitalization may be required.
7. When should I seek medical attention?
If you or a loved one experience severe symptoms, such as persistent high fever, difficulty breathing, or worsening cough, it is advisable to seek medical attention promptly. Healthcare professionals can provide a proper diagnosis and offer appropriate treatment recommendations.
Conclusion:
HMPV is a respiratory virus that is spreading in the United States. It can cause symptoms similar to the common cold or more severe respiratory infections. By practicing good hygiene, taking preventive measures, and seeking medical attention when necessary, we can minimize the spread and impact of HMPV. Stay informed and take care of your health and well-being.
Rheumatoid Arthritis: A Comprehensive Overview of Pathogenesis, Clinical Features, Diagnosis, and Treatment
Rheumatoid arthritis (RA) is a chronic autoimmune disease characterized by persistent inflammation of the synovial joints. It affects approximately 1% of the global population and can lead to significant disability if left untreated. This article provides a detailed review of the pathogenesis, clinical features, diagnosis, and treatment options for rheumatoid arthritis.
1. Introduction:
Rheumatoid arthritis is a systemic autoimmune disorder primarily affecting the joints. It is characterized by chronic inflammation of the synovial membranes, leading to progressive destruction of articular cartilage and bone. The disease often leads to joint deformity, functional impairment, and a reduced quality of life for affected individuals.
2. Pathogenesis:
Rheumatoid arthritis (RA) is a chronic autoimmune disease characterized by inflammation of the joints. It primarily affects the synovial lining of the joints, leading to pain, swelling, stiffness, and eventually joint deformity and functional impairment. The pathogenesis of rheumatoid arthritis is complex and involves multiple genetic, environmental, and immunological factors.
*Genetic Factors:
There is evidence to suggest a genetic predisposition to rheumatoid arthritis. Certain genes, such as the human leukocyte antigen (HLA) genes, specifically the HLA-DRB1 allele, are strongly associated with an increased risk of developing RA. However, having these genetic markers does not guarantee the development of the disease, indicating that other factors play a role as well.
*Environmental Factors:
Various environmental factors have been implicated in the development of rheumatoid arthritis. These include smoking, which is the most significant environmental risk factor for RA. Exposure to certain infections, such as Epstein-Barr virus and Porphyromonas gingivalis, a bacterium involved in gum disease, has also been associated with an increased risk of developing RA.
*Immune System Dysfunction:
The immune system plays a critical role in the pathogenesis of rheumatoid arthritis. In individuals susceptible to the disease, an initial trigger, such as an infection or environmental factor, activates the immune system inappropriately. This leads to a cascade of events involving both innate and adaptive immune responses.
*Inflammatory Response:
The activated immune cells release pro-inflammatory cytokines, such as tumor necrosis factor-alpha (TNF-α), interleukin-1 (IL-1), and interleukin-6 (IL-6). These cytokines promote inflammation and recruit additional immune cells to the joints, causing synovial tissue inflammation and subsequent destruction of cartilage and bone.
*Autoantibody Production:
In rheumatoid arthritis, the immune system produces autoantibodies, specifically rheumatoid factor (RF) and anti-cyclic citrullinated peptide (anti-CCP) antibodies. These autoantibodies target self-proteins, such as immunoglobulins and citrullinated peptides, forming immune complexes that contribute to the inflammatory response and joint damage.
*Synovial Hyperplasia:
The chronic inflammation in the synovial lining of the joints leads to synovial hyperplasia, characterized by increased cell proliferation and infiltration of immune cells. The hyperplastic synovium, known as pannus, invades the adjacent cartilage and bone, causing erosion and destruction.
*Osteoclast Activation:
Activated immune cells and inflammatory cytokines stimulate the production and activation of osteoclasts, cells responsible for bone resorption. Osteoclast activation leads to the destruction of the underlying bone in affected joints, further contributing to joint deformities and functional impairment.
Overall, the pathogenesis of rheumatoid arthritis involves a complex interplay of genetic, environmental, and immunological factors. While the exact trigger and mechanisms underlying the disease are not yet fully understood, ongoing research aims to shed light on the pathogenic pathways involved. Understanding the pathogenesis of RA is crucial for the development of targeted therapies and interventions to better manage this chronic autoimmune condition.
3. Clinical Features:
The clinical presentation of rheumatoid arthritis varies among individuals, but commonly includes joint pain, swelling, stiffness, and functional limitations. Typically, RA affects the small joints of the hands and feet symmetrically. Systemic symptoms such as fatigue, malaise, and low-grade fever may also be present. Extra-articular manifestations can involve other organs, such as the skin, eyes, lungs, and heart.
4. Diagnosis:
Diagnosing rheumatoid arthritis requires a combination of clinical assessment, laboratory tests, and imaging studies. Key diagnostic criteria include the presence of symmetric joint swelling and morning stiffness lasting for at least one hour. Blood tests for rheumatoid factor (RF) and anti-cyclic citrullinated peptide (anti-CCP) antibodies are helpful in confirming the diagnosis. Imaging modalities like X-rays and ultrasound can detect joint erosions and synovitis.
5. Treatment:
The management of rheumatoid arthritis aims to control disease activity, relieve symptoms, and prevent joint damage. Treatment strategies often involve a multidisciplinary approach, including pharmacological interventions, physical therapy, and patient education. Nonsteroidal anti-inflammatory drugs (NSAIDs) and corticosteroids provide symptomatic relief, while disease-modifying anti-rheumatic drugs (DMARDs) such as methotrexate and biologic agents target the underlying immune response. Early intervention and aggressive treatment have been shown to improve outcomes and slow disease progression.
6. Future Perspectives:
Ongoing research in rheumatoid arthritis focuses on identifying novel therapeutic targets and developing personalized treatment strategies. Advances in biologic agents, targeted synthetic DMARDs, and regenerative medicine hold promise for improved disease control and long-term outcomes. Additionally, lifestyle modifications, such as regular exercise and smoking cessation, can play a crucial role in the management of RA.
Conclusion:
Rheumatoid arthritis is a chronic autoimmune disorder characterized by joint inflammation and destruction. Early diagnosis and aggressive treatment are essential for optimal outcomes. A comprehensive understanding of the pathogenesis, clinical features, diagnostic approaches, and treatment options can guide healthcare professionals in effectively managing this complex disease and improving the quality of life for patients with rheumatoid arthritis.
Wednesday 31 May 2023
Real-Time PCR: Unveiling the Importance of CT Value in Infectious Disease Treatment
Introduction:
Infectious diseases continue to pose a significant threat to public health globally. The ability to rapidly and accurately diagnose these diseases is crucial for effective treatment and containment. Real-time polymerase chain reaction (PCR) has revolutionized the field of infectious disease diagnostics, allowing for precise and timely detection of pathogens. One of the key parameters derived from real-time PCR analysis is the CT value, which holds immense importance in guiding treatment decisions and monitoring disease progression. This article aims to explore the concept of real-time PCR and delve into the significance of the CT value in the context of infectious disease treatment.
Understanding Real-Time PCR:
Polymerase chain reaction (PCR) is a laboratory technique used to amplify a specific segment of DNA or RNA from a complex mixture. Traditional PCR involves multiple cycles of amplification and requires a separate step for detecting the amplified product post-amplification. Real-time PCR, also known as quantitative PCR (qPCR), is an advanced version that allows the detection of amplified DNA or RNA in real-time as the reaction progresses. This real-time monitoring is achieved by incorporating fluorescent dyes or probes into the reaction mixture.
Real-time PCR is a highly sensitive and specific technique that enables the rapid identification and quantification of nucleic acids. It is widely employed for diagnosing various infectious diseases, including viral, bacterial, and fungal infections. By targeting specific regions of the pathogen's genetic material, real-time PCR can confirm the presence of the infectious agent with high accuracy.
The Significance of the CT Value:
The CT value, also referred to as the cycle threshold or quantification cycle (Cq), is a crucial parameter derived from real-time PCR analysis. It represents the cycle number at which the fluorescence signal generated by the amplification reaches a specific threshold level. The CT value is inversely proportional to the amount of target nucleic acid initially present in the sample. A lower CT value indicates a higher initial target concentration, while a higher CT value suggests a lower initial target concentration.
In the context of infectious disease treatment, the CT value holds significant importance for several reasons:
1. Diagnostic Potential:
The CT value provides a quantitative measure of the pathogen's load in a clinical sample. By comparing the CT value obtained from a patient's sample to established reference ranges, clinicians can determine whether an infection is present, aiding in accurate diagnosis.
2. Monitoring Disease Progression:
During the course of an infection, the CT value can serve as an indicator of disease progression or response to treatment. A decreasing CT value over time suggests a reduction in pathogen load, indicating successful treatment. Conversely, an increasing CT value may indicate treatment failure or the emergence of drug resistance.
3. Treatment Guidance:
The CT value can help guide treatment decisions, particularly in the case of viral infections. Different viral infections have varying levels of virulence and response to antiviral medications. By monitoring the CT value over time, clinicians can assess the effectiveness of antiviral therapy and make adjustments accordingly.
4. Contagiousness Assessment:
The CT value can provide insights into the contagiousness of an individual infected with a particular pathogen. Lower CT values indicate higher viral loads and suggest that the patient may be more contagious. This information can assist in implementing appropriate infection control measures to limit the spread of the disease.
5. Prognostic Indicator:
In some cases, the CT value has been correlated with the severity of the disease and patient outcomes. Studies have shown that a higher CT value at the time of diagnosis may be associated with a milder course of illness, while a lower CT value may indicate a higher risk of complications or adverse outcomes.
Conclusion:
Real-time PCR has revolutionized infectious disease diagnostics, providing rapid and accurate detection of pathogens.
Saturday 27 May 2023
What is Blood Culture in ID Diagnostics ?
Friday 26 May 2023
Understanding Enteric Fever: Causes, Symptoms, and Treatment
Introduction:
Enteric fever, also known as typhoid fever, is a bacterial infection primarily caused by Salmonella enterica serotype Typhi (S. Typhi) and, less commonly, by Salmonella enterica serotype Paratyphi (S. Paratyphi). It is a significant public health concern, particularly in regions with poor sanitation and limited access to clean water. In this blog, we will explore the causes, symptoms, diagnosis, and treatment options for enteric fever.
1. Causes of Enteric Fever:
Enteric fever is primarily caused by consuming food or water contaminated with the Salmonella bacteria. The bacteria can survive in fecal matter, and transmission occurs through the oral-fecal route. Common causes of enteric fever include:
a) Contaminated Water: Drinking water contaminated with the Salmonella bacteria, typically from poor sanitation or sewage systems, is a significant source of infection.
b) Contaminated Food: Consuming food prepared under unhygienic conditions or using contaminated water for washing can lead to the ingestion of Salmonella bacteria.
c) Carrier Individuals: Individuals who have recovered from enteric fever but continue to harbor the bacteria in their gallbladder can be carriers and spread the infection to others.
2. Symptoms of Enteric Fever:
Enteric fever is characterized by a wide range of symptoms, which can vary in severity. Common symptoms include:
a) High Fever: Sustained high fever, often gradually increasing over a few days, is a hallmark of enteric fever.
b) Gastrointestinal Symptoms: Abdominal pain, diarrhea, or constipation are common gastrointestinal symptoms associated with enteric fever.
c) Headache and Body Aches: Intense headache, body aches, and general malaise are frequently experienced by individuals with enteric fever.
d) Weakness and Fatigue: Persistent weakness and fatigue are common, leading to a significant impact on daily activities.
e) Rose Spots: A distinctive rash of rose-colored spots may appear on the trunk or abdomen in some individuals.
3. Diagnosis of Enteric Fever:
Prompt and accurate diagnosis is crucial for effective management of enteric fever. Common diagnostic methods include:
a) Blood Culture: Isolating the bacteria from a blood sample is the gold standard for diagnosing enteric fever.
b) Stool Culture: Testing a stool sample can help identify carriers or individuals with milder symptoms.
c) Serological Tests: Antibody-based tests, such as the Widal test, may be used to detect specific antibodies against Salmonella.
4. Treatment of Enteric Fever:
Enteric fever requires medical intervention, and treatment typically involves the following:
a) Antibiotics: Antibiotics like fluoroquinolones or third-generation cephalosporins are commonly prescribed to kill the Salmonella bacteria. However, antibiotic resistance is a growing concern, and treatment choices may vary based on local resistance patterns.
b) Supportive Care: Adequate hydration, rest, and maintaining a balanced diet are essential for recovery. Over-the-counter pain relievers can help manage fever and body aches.
c) Prevention: Vaccination against S. Typhi is available and recommended in areas with a high incidence of enteric fever. Additionally, practicing good hygiene, including handwashing and consuming safe food and water, is crucial in preventing the spread of the disease.
Conclusion:
Enteric fever, caused by Salmonella bacteria, is a significant health issue in many parts of the world. Early diagnosis and appropriate treatment with antibiotics are essential for a successful recovery. Additionally, preventive measures such as vaccination, maintaining good hygiene practices, and ensuring access to safe food and water play a vital role in reducing the incidence of enteric fever. If you experience symptoms suggestive of enteric fever, it is important to consult a healthcare professional for proper diagnosis and treatment.
Thursday 25 May 2023
Community acquired Pneumonia - What should you know ?
Wednesday 24 May 2023
Hypertension - A silent killer ?
Health Tips for Summer and Monsoon - Must know points
Saturday 15 April 2023
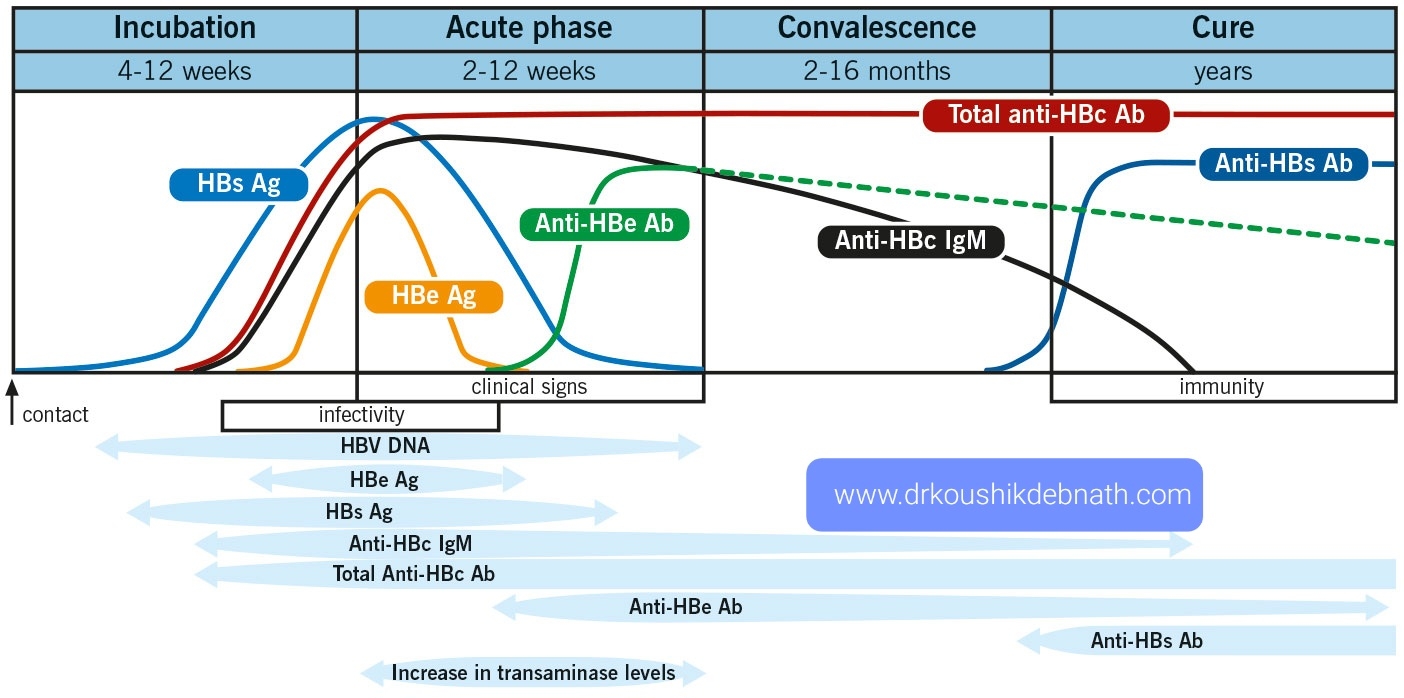
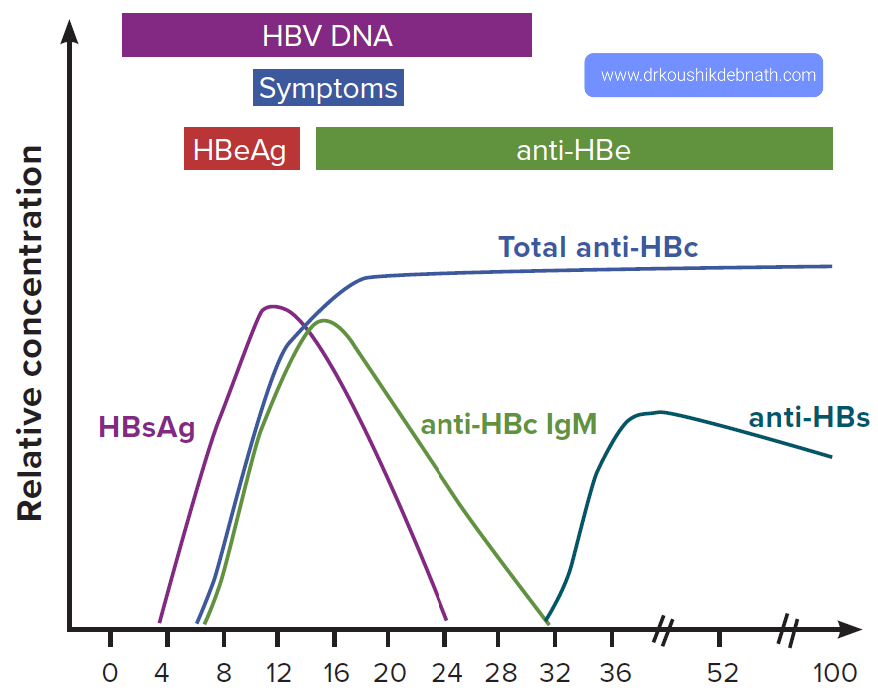
Hepatitis B - A Vaccine preventable serious Liver Infection
Acute hepatitis B virus infection:
Thirty percent of patients with acute hepatitis B develop icteric hepatitis, while roughly seventy percent have subclinical or anicteric hepatitis. Patients with underlying liver disease or other hepatitis viruses may have a more severe case of the disease.
One to six months pass during the incubation phase. During the prodromal stage, a syndrome resembling serum sickness may appear, followed by constitutional symptoms, anorexia, nausea, jaundice, and discomfort in the right upper quadrant. In most cases, the symptoms and jaundice go away after one to three months. A rare condition, cute liver failure affects 0.1 to 0.5 percent of patients.
Acute hepatitis with HBsAg positivity can also be diagnosed as:
(1) Acute hepatitis B
(2) Chronic hepatitis B exacerbations, such as acute hepatitis brought on by drugs and other toxins in a chronic hepatitis B infected person, reactivation of chronic hepatitis B, or superinfection of a chronic hepatitis B infection with hepatitis C, A, E, or D virus.
Alanine and aspartate aminotransferase levels (ALT and AST) are elevated during the acute phase of acute hepatitis B; values up to 1,000 to 2,000 IU/L are typically seen during this phase, with ALT being higher than AST. The serum levels of lactic dehydrogenase and alkaline phosphatase are typically only slightly elevated (less than threefold). Both the direct and indirect fractions of the bilirubin are variablely elevated. Patients with an-icteric hepatitis may have normal serum bilirubin levels. Except in cases of chronic, severe disease, serum albumin rarely decreases. The best prognosis predictor is the prothrombin time.
Normalisation of serum aminotransferases takes one to four months to happen in patients who make a full recovery. Persistent elevation of serum ALT for more than six months may indicate progression to chronic hepatitis.
- Precore mutants have mutations in the precore region, which abolishes HBeAg production, or in the core promoter region, which downregulates HBeAg production. Despite possibly producing anti-HBe and anti-HBc antibodies, these patients do not produce HBeAg.
- The second group of so-called escape mutants (due to mutations in a determinant of S gene preventing them from being neutralised by the anti-HBs) is seen in some infants born to HBeAg positive mothers and in liver transplant patients who have received combined immunisation with anti-HBV immunoglobulin and vaccine. This has no effect on viral replication; in fact, such cases are more difficult to treat and have a higher risk of turning into cirrhosis.
- HBeAg and HBsAg may both be suppressed by co-infection with HCV.
- HBcAb is occasionally the only serological marker that can be found. This could be either because of Co-infection with HCV or HIV, Remote infection, "Window" period between HBsAg and HBsAb, False positive test result - HBcAb is marker most prone to false positives or Resolved HBV with diminishing anti-HBs levels.
- Regardless of ALT levels, HBeAg status, or HBV DNA levels, treatment for all adults, adolescents, and kids with CHB and signs of compensated or decompensated cirrhosis should be prioritised.
- Regardless of HBeAg status, treatment is advised for adults with CHB who do not have cirrhosis but are older than 30 (in particular), have persistently abnormal ALT levels, and show evidence of high-level HBV replication (HBV DNA >20 000 IU/mL).
- In people without signs of cirrhosis, with persistently normal ALT levels, and with low levels of HBV replication (HBV DNA 2000 IU/mL), regardless of HBeAg status or age, antiviral therapy is not advised and can be postponed.
- In the absence of HBV DNA testing, treatment can be postponed in HBeAg-positive people 30 years of age or younger with persistently normal ALT levels.
- All CHB patients need to be monitored regularly, but it's especially important for those who don't currently fit the guidelines for whether or not to receive treatment, to find out if antiviral therapy will ever be necessary to stop the progression of liver disease. These people include those under 30 years old without cirrhosis who have HBV DNA levels greater than 20,000 IU/mL but persistently normal ALT.
- The NAs with a high barrier to drug resistance (tenofovir or entecavir) are advised for all adults, adolescents, and children aged 12 years or older for whom antiviral therapy is indicated.
- Tenofovir may be preferred as the medication of choice in women of childbearing age in the event of pregnancy. Pregnancy is not advised when using entecavir.
- Patients with a risk of developing Entecavir resistance who have taken lamivudine are advised to use tenofovir instead.
- Children between the ages of 2 and 11 should not take entecavir.
- Entecavir may be preferred over Tenofovir in Age > 60, history of fragility fractures or osteoporosis; use of other drugs that worsen bone density, altered renal function (eGFR 60 mL/min/1.73 m2, albuminuria > 30 mg/24 hr, moderate dipstick proteinuria, Low phosphate (2.5 mg/dL) or in patients receiving hemodialysis.
- Drugs with a low barrier to resistance (lamivudine, adefovir, or telbivudine) are available but not advised as they promote drug resistance. Tenofovir alafenamide fumarate (TAF) is the drug of choice in patients with reduced renal function or bone disease bone toxicities, where entecavir is contraindicated.
- HBV DNA levels (where HBV DNA testing is available), HBsAg, HBeAg, and ALT levels (and AST for APRI)
- Non-invasive tests (APRI score, FIB-4, or FibroScan) to determine whether fibrosis has gotten worse or whether cirrhosis has developed in people who didn't have it at the start.
- If receiving treatment, adherence needs to be checked frequently and at each appointment.
Monday 27 March 2023
Scrub Typhus - A potentially life threatening fever ?
What is scrub typhus ?
Orientia tsutsugamushi, an obligate intracellular gram-negative bacterium, is the source of the acute febrile illness known as scrub typhus. Although scrub typhus caused by other Orientia species has been reported in Africa, France, the Middle East, and South America, it is believed to be endemic to the tsutsugamushi triangle, which includes Asia, northern Australia, and islands in the Indian and Pacific Oceans. According to a recent systematic review from hospital-based studies in India, scrub typhus was the root cause of 25% of acute undifferentiated febrile illnesses.
O. tsutsugamushi transmitted by the bites of infected chiggars( trombiculid mite) has been linked in recent studies to acute encephalitis syndrome (AES) outbreaks in India, particularly in the northern states of Uttar Pradesh, Bihar, West Bengal, and Assam. Outbreaks of AES pose a major public health problem in India, predominantly affecting children.
Spectrum of Clinical Features-
All patients who exhibit an acute onset of fever and altered mental status are included in the broad definition of Acute Encephalitis Syndrome used for syndromic surveillance. Typical clinical features include fever with chills & rigor ,headache,bodyaches,muscle cramps,altered sensorium ,lymphadenopathy and rash .
The pathognomonic classical scrub typhus rash has been described as a dark scab like region at the site of the chiggar bite, popularly known as 'Eschar'.
Diagnostic Challenges-
Early diagnosis is essential for starting prompt, targeted treatment, which can lower scrub typhus complications and fatality rates. Due to the symptoms' similarity to those of other tropical infections that are endemic to the region and can also cause AES, such as dengue, chikungunya, malaria, and leptospirosis, clinical diagnosis can be difficult.
There are drawbacks to the current microbiological diagnostics for scrub typhus, which are typically based on IgM detection in serum samples or nucleic acid by PCR. IgM can persist for a long time after the onset of acute illness, and it can react with IgM from other cocirculating pathogens. IgM first appears in serum 5–6 days after the onset of illness .Therefore, it is challenging to determine O. tsutsugamushi as the cause in AES patients who also have microbiological evidence of another potential pathogen.
Patients with suspected neurologic scrub typhus do not undergo routine IgM detection in cerebrospinal fluid (CSF).The immunofluorescence assay has long been regarded as the gold standard in serologic testing, but its use is constrained by its high cost and difficult interpretation. Serologic tests' limitations in terms of cross-reacting and persistent antibodies may be addressed by PCR, but a positive result is only likely to occur during the bacteremia stage of infection .
Additionally, blood or eschar material are suggested samples for O. tsutsugamushi PCR, whereas it is unknown how sensitive PCR is to CSF.More than 50% of patients had anaemia, leukocytosis, thrombocytopenia, transaminitis, hypoalbuminemia, and uremia. Most patients' CSF tests showed lymphocytic pleocytosis and increased protein concentration.
Treatment-
Doxycycline 100mg twice daily x 10 days has been the drug of choice for most of the patients without having obvious comorbid conditions. Supportive therapy in terms of Paracetamol, Intravenous Fluids etc are often required. Comorbid conditions like Diabetes Mellitus, Pre-existing Nephropathy can lead to AKI like manifestations in selected group of patients. Hence a constant vigilant monitoring of serum creatinine, electrolytes along with CRP/Procalcitonin may be of importance to optimise the therapeutic outcome.
Sunday 5 March 2023
Typhoid vaccine price in India - Know why it is worth the cost
What is Typhoid Fever ?
A potentially fatal multisystemic infection known as enteric fever, also known as typhoid fever is caused primarily by Salmonella enterica serotype typhi and, to a lesser extent, paratyphi A, B, and C. ICD 10 code for enteric fever is now A01.00. Salmonella are motile enterobacteriaceae that can cause a number of different gastrointestinal infections. Typhoid, which is primarily caused by Salmonella enterica serotype typhi and, to a lesser extent, S enterica serotypes paratyphi A, B, and C, is the most dangerous of these. From a severe septic illness to minor cases of diarrhoea with low-grade fever, it can present in a wide range of ways. Fever, malaise, diffuse abdominal pain, and constipation are characteristics of the classic presentation. Typhoid fever that is left untreated can lead to delirium, obtundation, intestinal bleeding, bowel perforation, and death in less than a month.
It has grown more and more resistant to antibiotics over time. Extensively drug-resistant typhoid (XDR) was reported in Pakistan in 2016. Azithromycin, carbapenems, and tigecycline are the only antimicrobial classes that are still effective against these strains.
Conditions of poor sanitation, overcrowding, and social unrest favour the growth of typhoid. Typhoid fever is still endemic in developing nations, despite the fact that antibiotics have significantly decreased its prevalence in the developed world. It's possible that S paratyphi infections are becoming more common than S typhi infections. This might be brought on by the immunologic immaturity of a particular population as well as the insufficient protection against these pathogens offered by the current Typhoid vaccines. Most commonly, non-Typhoidal strains cause a mild, self-limiting gastroenteritis. Nevertheless Typhoid vaccines play a crucial role both in primary prevention and decreasing the disease severity in affected individuals.
Vaccines for prevention :
 |
| Courtesy : Dr Koushik's Medicare |
Typhoid fever can be prevented by two vaccinations. The first is a live, attenuated (weakened) vaccine, and the second is an inactivated (dead) vaccine. Which typhoid vaccine is ideal for you can be decided with the aid of your doctor. Typhoid vaccination that has been inactivated is given by injection. Children of 2 years of age and older may receive it. At least two weeks prior to departure, one dose is advised. For those who continue to be at danger, repeated doses every two years are advised.
Oral live typhoid vaccine administration (by mouth). Six years of age and older individuals may receive it. Every other day, one capsule is taken, making a total of four capsules. At least a week before departure, the last dose should be taken.About an hour before meals, each capsule should be taken whole (without chewing) with cold or lukewarm water. For those who continue to be at risk, a booster shot is required every five years. It's crucial to keep live typhoid vaccine capsules chilled (not frozen).
In developed countries most of the time routine typhoid immunisation is not advised, although the following situations may warrant administration of typhoid vaccines.
a) Tourists going to regions where typhoid is widespread. (NOTE: Typhoid vaccination is not 100% effective and is not a replacement for exercising caution while choosing foods and beverages.)
b) Individuals in close proximity to a typhoid carrier.
c) Employees in laboratories that handle Salmonella typhi bacterial culture and strains
The typhoid vaccine may be administered concurrently with other shots.
In 2023 typhoid vaccine price in India is around INR 1500-2500 based on the brands available. You can check the same on : https://www.apollopharmacy.in/medicine/typbar-tcv-pfs-injection-0-5ml
Typbar TCV Vaccine 0.5 ml. It includes sodium chloride and the purified Vi polysaccharide typhoid vaccine. Typhoid disease is prevented with it. A non-toxic and safe form of the causative bacteria's capsular specimen is injected into the body by Typbar TCV Vaccine, which prompts the body to produce antibodies and confers immunity. The body keeps track of this immune response to ensure that it is ready in the event that these bacteria invade again in the future.

-
Itchy skin can be attributed to different etiological agents. Amongst those the most common is Dermatophytes which implies superficial funga...
-
Antibiotics have been a wonderful invention in the evolution of modern medical treatments. The mortality and the morbidity due to diffe...
-
When winter had come can spring be far behind ? Well we all are gearing up to welcome spring which symbolises colour and fes...